- Healthcare 150
- Posts
- The Medicare Advantage Explosion, Agentic AI’s Next Wave, and Telehealth’s $1.4T Future
The Medicare Advantage Explosion, Agentic AI’s Next Wave, and Telehealth’s $1.4T Future
Today we explore the total medicare advantage enrollment throughout the years, agentic AI spending is expected to moderately increase in 2026, and the booming telehealth market to reach $1.4T by 2035.
Good morning, ! Today we explore the total medicare advantage enrollment throughout the years, agentic AI spending is expected to moderately increase in 2026, and the booming telehealth market to reach $1.4T by 2035.
Want to advertise in Healthcare 150? Check out our ad platform, here.
Know someone in the healthcare space who should see this? Forward it their way. Here’s the link.
— The Healthcare150 Team
DATA DIVE
Medicare Advantage: Growth Meets Margin Reality

Medicare Advantage (MA) has quietly become the center of gravity in U.S. healthcare financing. In 2025, 54% of Medicare beneficiaries — about 34.1 million people — were enrolled in MA plans, with enrollment expected to reach roughly 35 million in 2026.
But the growth story is entering a new chapter. Plan supply is shrinking, falling from 3,998 plans in 2023 to 3,373 in 2026, even as enrollment continues to rise. Insurers are shifting from aggressive expansion to portfolio rationalization, pulling back from lower-density markets and focusing on regions where scale and risk-adjusted economics work.
Meanwhile, market concentration remains high: UnitedHealthcare and Humana control ~46% of MA enrollment.
The takeaway: Medicare Advantage is still expanding, but margin discipline — not growth alone — is becoming the defining competitive advantage. (Read the Full Report Here)
PRESENTED BY JUNIPER SQUARE
The private markets have evolved beyond traditional closed-end funds. More GPs are launching new fund structures tailored to different investor profiles with different liquidity expectations and faster operating cadences.
That shift changes what “good operations” looks like. Investor onboarding, servicing, reporting, and communications cannot be treated as a series of handoffs across point solutions, as disconnection creates friction, inconsistency, and slower decision-making.
With all these new fund structures in play, the operating model decides who scales and who stalls. Connected fund and investor data turns execution into a competitive advantage — giving teams the speed, precision, and confidence to scale without adding friction.
Download the report to understand what’s driving the rise of new fund structures and the operational implications for GPs.
Supporting our sponsors supports our free newsletters. Please support our sponsors!
HEALTHTECH CORNER
Agentic AI Spending Is Coming, But Gradually
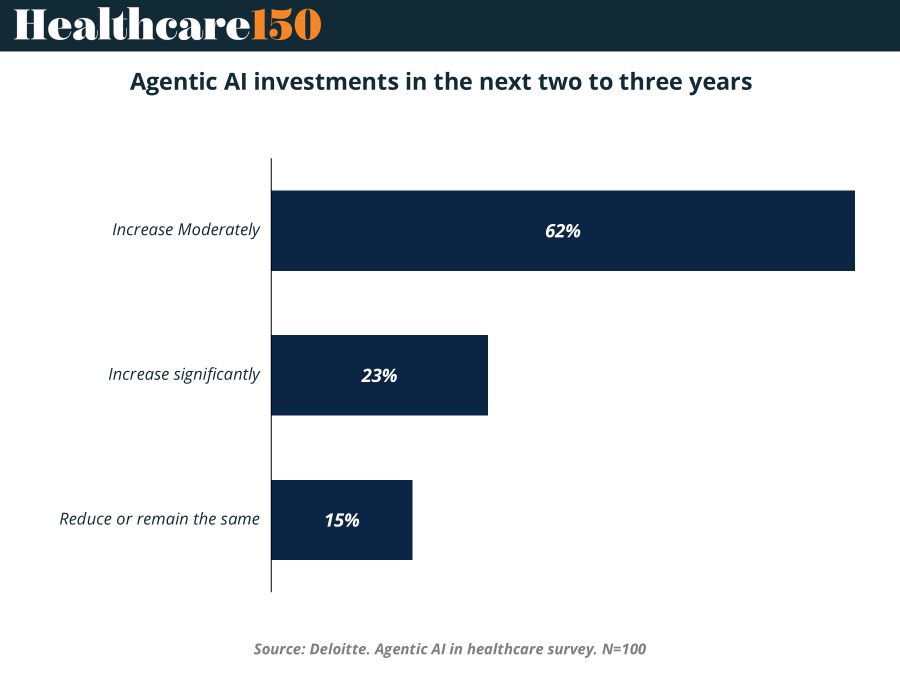
Healthcare executives expect meaningful investment in agentic AI, but the pace will be evolutionary rather than explosive. In a recent Deloitte survey of 100 healthcare leaders, 62% expect spending on agentic AI to increase moderately over the next two to three years, while 23% anticipate a significant increase. Only 15% expect spending to remain flat or decline.
The distribution is revealing. Most systems are preparing for adoption, but few are ready to scale aggressively. This suggests that healthcare organizations are treating agentic AI as an operational capability to be tested and integrated, not a technology to deploy overnight.
For investors and operators, the signal is clear. The next phase of AI in healthcare will likely be defined by incremental integration into workflows such as clinical documentation, revenue cycle, and care coordination. Capital will favor platforms that can prove reliability inside existing systems rather than standalone AI tools promising radical disruption.
The opportunity is large, but the deployment curve will likely follow healthcare’s usual pattern. Slow validation first, then rapid scale once the operational case is proven. (More)
COMPLIANCE CORNER
Governance in 2026: Dual Federal–State Compliance Currents
Healthcare compliance governance is entering a paradoxical phase. Federal regulators like CMS signal selective deregulation—softening oversight on Medicare Advantage and ACA subsidies—while tightening mandates on prior authorization transparency, data interoperability, and privacy protections.
At the same time, states are expanding oversight, introducing mandates on pharmacy benefit managers (PBMs), substance use disorder coverage, and dual premium filings amid federal subsidy uncertainty.
Why it matters: This dual regulatory pressure requires compliance programs capable of navigating divergent federal and state frameworks. Real-time monitoring, algorithm transparency, and enterprise data governance are becoming baseline expectations. Prior authorization timelines and denial reporting now demand robust auditing infrastructure and greater public accountability.
Key shift: Health plans and providers must automate compliance using AI and machine learning to meet accelerated timelines and expanding reporting mandates. Updated ONC rules emphasize transparency in predictive tools and decision logic, reinforcing compliance’s technological dimension.
Bottom line: Compliance governance is no longer just policy oversight. It requires dynamic, multi-jurisdictional infrastructure. Boards must prioritize data integrity, audit rigor, and whistleblower readiness to sustain a resilient culture of compliance. (More)
COMPETITIVE LANDSCAPE SNAPSHOT

TREND TO WATCH
Telehealth’s Trillion-Dollar Trajectory

Telehealth is moving from pandemic necessity to core healthcare infrastructure — and the growth curve reflects it.
According to Precedence Research, the global telehealth market is projected to expand from $196.8B in 2025 to nearly $1.37T by 2035, representing more than a 6x increase over the decade and one of the fastest growth rates across healthcare services.
Several forces are driving the shift. Virtual care adoption has normalized, while Remote Patient Monitoring (RPM) and chronic care management are expanding telehealth’s role across primary care, behavioral health, specialty care, and post-acute services.
Meanwhile, payers and employers are leaning into telehealth as a tool for cost containment, earlier intervention, and reduced emergency utilization.
Bottom line: telehealth is no longer a digital health niche — it’s becoming a foundational layer of modern care delivery. (More)
“The first wealth is health.”
Ralph Waldo Emerson


